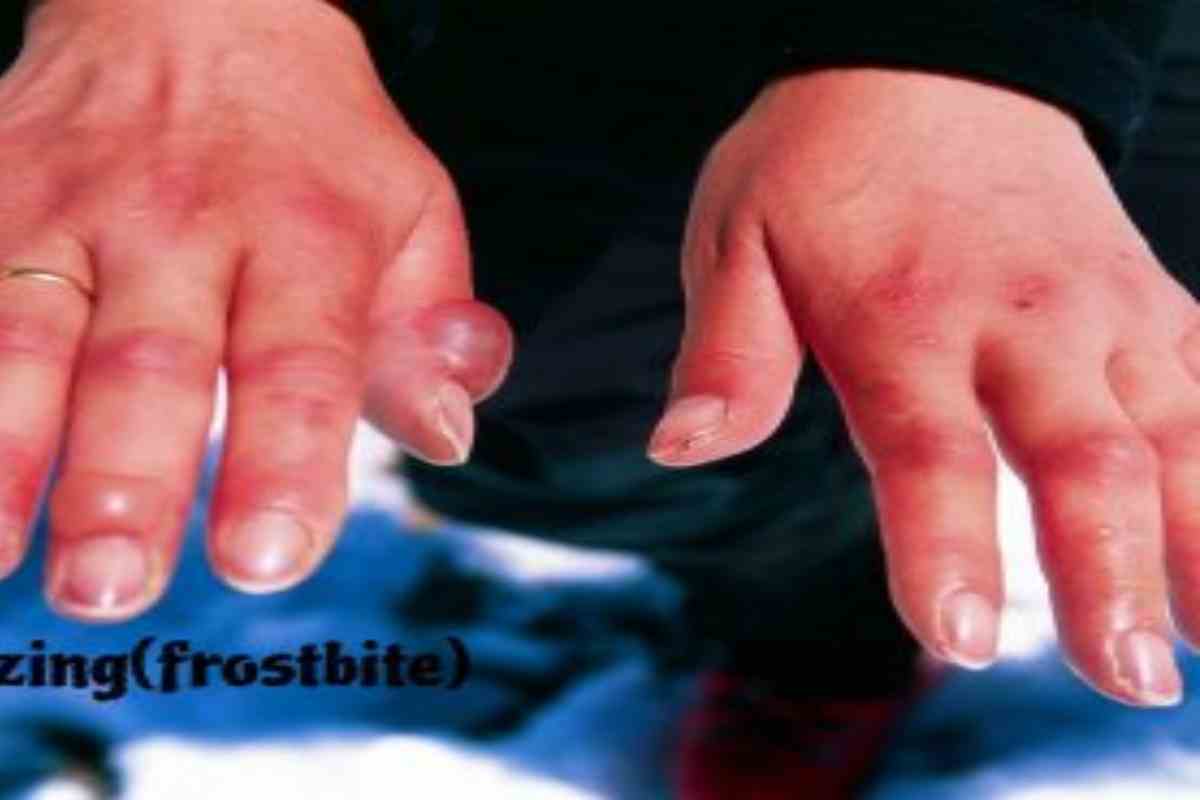
Freezing
Freezing (in English, frostbite ) is tissue damage caused by prolonged exposure to extreme cold. The initial stages of the phenomenon are superficial and do not cause permanent injuries; severe frostbite, however, requires medical attention, as it destroys underlying skin tissues and blood vessels.
The effects can be temporary (superficial frostbite) or permanent if complications arise, such as damage to muscles, bones, nerves, infections, and gangrene. Freezing Frostbite can sometimes replace by systemic hypothermia (or frostbite ), which affects the whole organism.
Table of Contents
Causes
At temperatures of 0 ° C or below, the blood vessels under the skin begin to narrow, and the blood is diverted from the extremities to the vital organs through the action of the glomus bodies (the glomus is a component of the dermis, involved in the regulation of body temperature ).
The same reaction can induce by exposure to strong winds and severe atmospheric conditions (e.g., snowstorms). Again, vasoconstriction helps maintain body temperature and prevent heat loss.
When the body exposes to cold for long periods, its protective strategy reduces blood flow to deficient levels in some areas as blood redirect away from the body’s extremities.
Fluids in the tissues freeze and form ice crystals, which can cause severe damage to the site. In addition, if blood flow cannot restore, it deprives cells of oxygen, eventually leading to tissue death (gangrene).
Degrees of Freezing
First-degree Freezing
The initial stages of frostbite affect only the skin’s surface, and the affected area is usually not permanently damaged. At the onset, numbness, tingling, itching, and pain occur in the affected area. Next, the skin becomes cold, numb, and pale due to impaired blood circulation. Mild forms of frostbite can resolve with the transfer of the patient to a warm place and with first aid measures.
Second-Degree Frostbite
If exposure to low temperatures continues, the frostbite extends to the epidermis and dermis but does not involve the deep tissues. As a result, the skin turns blue-white and hardens to the touch. Medical intervention is required to ensure that no permanent damage occurs.
With warming, the skin becomes red, swollen, itchy, and sore, and after 1-2 days, blisters or blisters appear. Second-degree injuries heal within a month, but the area can become permanently numb.
Third and Fourth-Degree Frostbite
Frostbite becomes more and more severe and leads to further damage involving muscles, tendons, blood vessels, and nerves. An inflammatory process establishes by the immune cells’ intervention, which temporarily compromises, and in severe cases, definitively, the functionality of the area involved.
As the skin thaws, the blisters fill with blood and turn into thick purplish-black crusts, while hurt to nerve endings can cause permanent loss of sensation. Fourth-degree injuries occur when frozen tissue begins to necrotize. Extreme frostbite may result in the need for surgery or amputation to remove necrotic tissue.
Symptoms
For further information: Freezing Symptoms
Symptoms of frostbite are varied, but common warning signs include numbness, burning, and pain in the area. If exposure to cold continues, tingling may result in loss of sensitivity to touch; with the aggravation of frostbite, the pain begins to fade until it disappears.
Other typical signs of frostbite include:
Decreased oxygen at the cellular level ( anoxia );
Edema ;
Bruising ;
Formation of blisters or bubbles
Tissue necrosis.
The body parts most inclined to frostbite are the nose, earlobes, fingers, and toes, as they are more exposed. In mild cases, full recovery is possible with quick medical intervention. The most significant consequences occur in tissues that freeze, thaw and re-freeze.
Risk Factors
F frostbite risk factors include conditions that cause vascular damage and circulation problems, such as diabetes and Raynaud’s phenomenon. Frost is not a common problem, but some people who practice winter and high altitude sports (such as mountaineers and skiers) or work extensively in extreme weather conditions (sailors and lifeguards) should take precautions.
In those contexts, the identical elements which could result in frostbite (cold temperatures, inappropriate garb, wet clothing, freezing wind, and many others.) can make contributions to hypothermia.
Treatment
Treatment of frostbite harm depends on the severity of the condition. If medical assistance is not readily available, seeking a stable, warm environment is helpful. However, it is essential to recall that excessive movement of frozen tissue can cause further injury – friction can destroy already broken skin and increase the risk of infection.
For this reason, rubbing or applying physical force in an attempt to heal the affected area can be harmful. You can heat in these ways:
Passive warming: involves the use of body heat or room temperature. Passive heating includes wrapping in blankets to keep frozen parts or moving to warmer environments. The patient should not use direct heat sources, such as stoves, fireplaces or campfires, as they can affect burns (facilitated by the reduced or absent sensitivity of the explored area). Replacing wet clothing with soft, dry clothing can stop further heat loss.
Active heating: the administration of direct heat to a person requires more equipment and could be challenging to perform in a non-hospital setting. Vigorous heating obtains by immersing the wounded tissue in a water bath at a 40-42 ° C temperature for about an hour. Heating peripheral tissues can dilate blood vessels and restore circulation to the area. However, the procedure is intensely painful and can increase the risk of heart arrhythmias.
Surgery
Debridement and amputation of necrotic tissue are generally postponed interventions, with exceptions for the appearance of signs of infection or gas gangrene. Thrombolytic drugs, which act as tissue plasminogen activators (tPA), may give to reduce the need for amputation. However, these agents can cause severe bleeding and are typically only used within 24 hours of exposure in particular situations.
Recovery and Long-Term Effects
A full recovery is possible if the frostbite does not damage the blood vessels. If not, the injuries can be permanent. Several long-term effects can follow freezing: transient or permanent changes in sensation, paraesthesia, persistent pain, and arthritis in the affected part of the body.
Conclusion
Freezing is tissue damage caused by prolonged exposure to extreme cold. The initial stages of the phenomenon are superficial and do not cause permanent injury. Severe frostbite, however, requires attention.